Reviewed By:
As new substances hit the market and old ones return, it can be hard to stay informed. Here's a look at how COVID-19 affected drug trends and what to watch for in 2021.
Table Of Contents
No matter how many new street drugs hit the market, it seems there’s always another on the horizon. Between semi-legal “supplements” and misused prescriptions, it’s not always easy to recognize a drug as dangerous. The COVID-19 pandemic has complicated the landscape as people look for an escape through anti-anxiety drugs. To help you stay informed, here’s a look at which drugs surged over 2020 and what to be aware of as the “club scene” returns.
Street Drugs to Watch in 2021
Social distancing led to a drop in popular club drugs like MDMA and cocaine in 202, while fueling a surge in alcohol, cannabis and anti-anxiety meds. Psychedelics like LSD, mushrooms and PCP also rose in popularity as people looked to mentally escape from a tough year.
Meanwhile, some dangerous pre-pandemic trends went unchecked. Fentanyl-laced drugs have continued to increase, and more benzodiazepines have made their way to the street. Here’s an overview of the biggest problem drugs of 2020, based on a global survey of use:
- Cannabis was most popular illicit drug of 2020, with a 46% increase in use among Americans
- MDMA/Ecstasy ranked last among the 11 drugs on the survey, dropping by 41% in the absence of festivals or nightclubs
- Without a club scene, cocaine fell by 38% and ketamine by 34%
- Psychedelics like magic mushrooms and LSD remained steady; about 20% of people said they increased their use
See additional resources in this download.
Emerging Street Drugs to Know
Below is an in-depth look at emerging drugs hitting the street. Some, like Phenibut and Kratom, were fueled by the pandemic, while others stand poised for a resurgence as nightclubs reopen and global travel resumes. Here’s what to know about each of these drugs, including the signs of an overdose and how to get help for addiction.
Phenibut
Also called: Anvifen, Fenibut, pbut, noofen, party powder

Originally developed by the Soviet Union for cosmonauts headed to space, Phenibut is an addictive anti-anxiety drug and nootropic still prescribed in some Eastern European countries. As an unscheduled substance in the United States, Phenibut is technically legal to use, but doctors may not prescribe it. Moreover, manufacturers may not sell it as having any health benefits. The drug made headlines recently after a report showing calls to poison control centers involving the drug have skyrocketed since 2018. Some cases involved deaths. Read more about Phenibut use, and why it’s on the rise.
How to spot it
Phenibut is typically sold as a dietary supplement, even though this claim is illegal. The pill itself often looks like a simple white capsule.
Fantasy (GHB)
Also called: G, Liquid Ecstasy, The New Ice

Gamma-Hydroxybutyrate, a drug users are now calling a ‘coma in a battle,’ has become a growing problem abroad. Queensland, Australia saw a 900% increase in seizures over the past four years, the Daily Mail reported, with multiple overdose deaths. The UK has also seen an increase in use across clubs. In the US, the drug was linked to the suspension of NBA player Tyreke Evans and hospitalization of actor Mischa Barton.
Sometimes prescribed as a treatment for narcolepsy under the name Xyrem, the drug causes hallucinations, drowsiness and excited or aggressive behavior. Signs of an overdose include slowed heart rate, lower body temperature, vomiting and nausea. Overdose can also lead to unconsciousness, seizures, coma, and even death.
How to spot it
GHB comes as a white powder, you may be more likely to see it in liquid form. Dissolved in another liquid, such as alcohol or juice, GHB is clear and may taste slightly salty.
Flakka (alpha-PHP)
Also called: Gravel, Zombie Drug, Bath Salts

Photo credit: DEA
A synthetic designer drug, Flakka is a stimulant that mimics the effects of the khat plant. It produces an amphetamine-like experience similar to Ecstasy, but the side effects can be far more dangerous. Users on Flakka have displayed violent aggression, self-harm and outright bizarre behavior. In one example, a user impaled himself on a fence; in another, a man ran through the streets naked, claiming someone had stolen his clothes. Users also report hallucinations, psychosis and delusions, drawing parallels to Flakka’s chemical cousin, bath salts.
Users may also experience physical harm, including increased body temperature, kidney failure and tachycardia. The combined effects have led the DEA to classify Flakka as a Schedule I narcotic, a category reserved for dangerous drugs that have no medical value, cause severe harm to the user, and are highly susceptible to physical dependence.
Although Flakka is not necessarily new to the street, with the first reports emerging in 2013, the drug has made an alarming comeback. According to a recent survey, as many as 1% of teens have tried the drug, raising a red flag for parents. Notably, many teens unwittingly ingested Flakka while intending to take MDMA or cocaine.
Have questions about addiction?
Call us at 855-430-9426 to speak with a recovery specialist.
How to spot it
On its own, Flakka comes in pink or white crystals, similar to bath salts. Like other synthetic drugs, it may come in pouches labeled as “plant food” or “phone screen cleaner.” When combined with other drugs, Flakka can be impossible to spot.
The bottom line: The potential side effects of Flakka make it one of the most dangerous drugs on the street. If you struggle with substance abuse or have a loved one who may be susceptible to using club drugs like cocaine or Molly, it’s important to know that Flakka may be among the “hidden” ingredients. To protect yourself, stay educated about drugs like Flakka and seek professional help for addiction.
Kratom
Also called: Herbal speedball, biak biak, ithang, thorn

A psychoactive herb made from the Mitragyna speciosa tree in Southeast Asia, kratom has made its way into gas stations, bodegas and convenience stores throughout the United States. Unregulated by the federal government, kratom has even appeared at farmers’ markets and in specialty health stores, promoting a narrative that the drug has medicinal value.
However, the FDA is quick to dispute that notion, issuing a warning against using kratom in a recent statement: “There are no FDA-approved uses for kratom, and the agency has received concerning reports about the safety of kratom. The FDA…continues to warn consumers not to use any products labeled as containing the botanical substance kratom or its psychoactive compounds, mitragynine and 7-hydroxymitragynine.”
The potential negative effects of kratom, which can include nausea, vomiting, liver damage and a high risk of addiction, have led eight US states and 18 countries to ban or regulate the substance. Other municipalities have instituted their own bans.
How to spot it
Derived from a green plant, kratom is typically ground up and put into capsules or brewed as a beverage. It might look like a green powder or loose-leaf tea.
To better understand the uses, side effects and regulation of kratom, check out these articles:
A Complete Guide to Kratom
Is Kratom Legal? Kratom Legality by State
Fentanyl
Also called: Apache, China Girl, Dance Fever, Poison, Blue Dolphin, Fire Birria (Fentanyl mixed with heroin), Facebook (Fentanyl and heroin in pill form), Speedball (Fentanyl mixed with cocaine), Goofball (Fentanyl mixed with meth)
Although the opioid crisis is unfortunately not a new one, the emergence of fentanyl has made it more dangerous. A powerful synthetic opioid up to 100 times more potent than morphine, fentanyl caused more than 30,000 deaths in 2018 — up from 3,000 deaths in 2013.
Given the low cost of production and low detection rate, officials expect these numbers to worsen in 2020. Dealers are also cutting the powder into an increasing number of street drugs. Fentanyl now routinely appears in cocaine, meth, MDMA, and benzodiazepines like Xanax and Etizolam. Lacing fentanyl into these drugs makes them cheaper to produce, but puts users at far greater risk of overdose.

Fatal dose of fentanyl. Photo credit: DEA
Because the chemical compounds of lab-produced drugs can change as new analogs hit the street, even online “testing kits” may not always detect fentanyl.
How to spot it
In its pure form, fentanyl is an unassuming white powder. However, you aren’t likely to see it when combined with other drugs. More likely, you’ll notice the symptoms. If you experience drowsiness, confusion, nausea, slowed breathing, sweating, and stiff or rigid muscles, dial 911 immediately.
Get the DEA Fentanyl Fact Sheet
Carfentanil
Also called: Wildnil, Serial Killer
An analog of fentanyl, carfentanil is making the opioid crisis even more deadly. Used primarily to sedate large animals like elephants and horses, carfentanil is one of the most potent drugs known in the United States. Just 0.02 mg — a trace amount — can trigger a fatal overdose. In fact, carfentanil is so dangerous that those who handle it must wear protective gear to prevent it from becoming absorbed by the skin.
So why do dealers use it? Ominously, for the same reason they use fentanyl: it’s less expensive and more potent than heroin, allowing illicit manufacturers to produce and sell greater amounts at lower costs. As with fentanyl, carfentanil is cut with other substances and sold as Xanax, Oxycontin, cocaine, MDMA and other drugs.
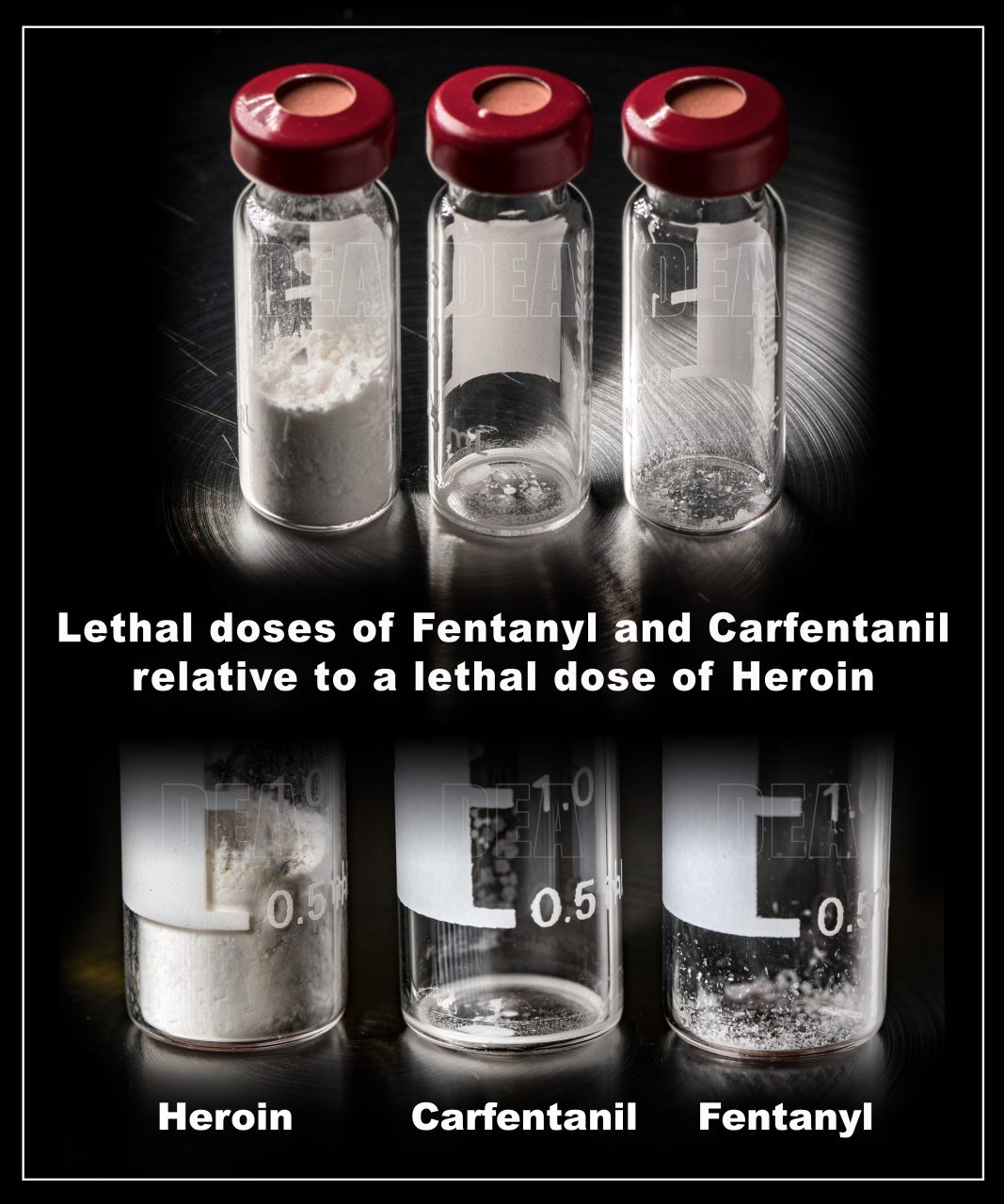
Photo credit: DEA
How to spot it
As with fentanyl, users aren’t likely to know they’ve taken carfentanil until after ingesting it. Symptoms begin within minutes and may include respiratory arrest, clammy skin and shallow breathing. Again, dial 911 immediately if you recognize any of these symptoms.
Get the DEA Carfentanil Safety Alert
Gabapentin
A multi-purpose drug used primarily to treat seizures and general nerve pain, gabapentin has only recently become a concern on the street. Recreational users take the drug to intensify an opioid high or as an opioid substitute. This makes it a worrisome newcomer in areas already plagued by heroin and prescription drug abuse.
As Rachel Vickers Smith, PhD, MPH, assistant professor in the University of Louisville School of Nursing, told US Pharmacist,“People are looking for other drugs to substitute for opioids, and gabapentin has filled that place for some. It has been easy to get a prescription for gabapentin and it’s very cheap.”
Widespread availability is part of the growing problem. Gabapentin is now the fourth-most prescribed drug in the United States as doctors use it to treat everything from restless leg syndrome to generalized anxiety disorder. As pharmacists spot increasing signs of abuse, a number of states have issued cautions. Eight of them, including New Jersey, have required that gabapentin prescriptions be reported to state officials. The FDA issued its own warning in December 2019 about potential serious breathing problems that can result when combining gabapentin with other opioids.
How to spot it
Gabapentin comes in pill or capsule form and is typically white or yellow. However, the drug may also be combined with other substances, including marijuana, cocaine or other opioids.
The bottom line: if your doctor prescribes gabapentin, you have little to worry about. On its own, the drug is not habit-forming and carries little risk of abuse. However, it should only be used as directed. If you have struggled with opioid addiction, gabapentin can interfere with your recovery and may have serious side effects.
Seeking Help for Addiction
If you or a loved one struggles with addiction, know that you are not alone. With an individualized approach to treatment, based on your unique history and needs, lifelong recovery is possible. The first step is learning your options. For dedicated medical attention while you detox, inpatient rehabilitation may be your best choice. Inpatient treatment gives you nurturing, professional support during withdrawal and the benefit of a supportive, temptation-free environment. This makes it easier to overcome physical dependence and make critical forward progress.
Outpatient treatment has proven equally effective for many people. With an outpatient program, you’ll receive the same professional support and medical guidance provided during inpatient treatment with the flexibility to spend evenings at home. You will also learn about ongoing resources to continue your recovery. These might include 12-step programs, cognitive behavioral therapy, and coping mechanisms to manage triggers for relapse and daily stress.
Whatever challenges you face in your own struggle with addiction, our team at Sprout Health Group can help. Call us at the number below to take the first step toward your recovery journey in 2021.
Have questions about addiction?Chat with one of our recovery specialists now.


